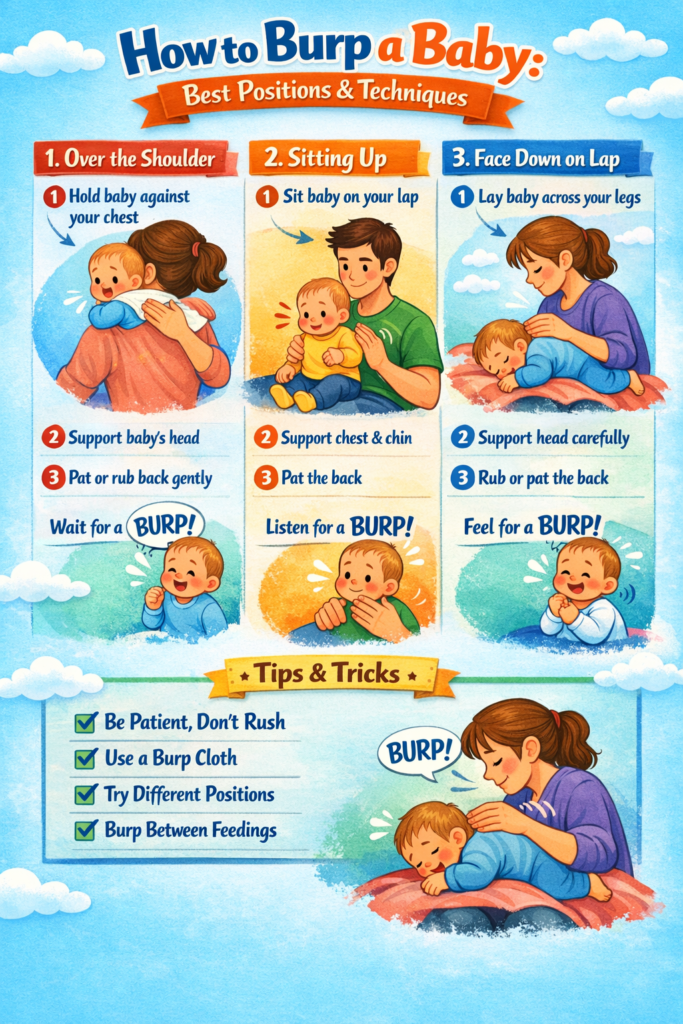
To burp a baby effectively, gently pat or rub their back using a cupped hand while supporting their head and neck. The three best positions are over your shoulder, sitting upright on your lap with chest support, or lying face down across your lap. Burp your baby halfway through a feeding and again at the end to release trapped air and prevent gas pain.
The Vital Role of Burping in Infant Digestion
Feeding a newborn, whether via breast or bottle, is one of the most fundamental bonding experiences for a parent. However, the process doesn’t end when the milk is gone. Burping is a mandatory extension of feeding time that directly impacts your baby’s comfort, sleep quality, and overall digestive health.
When infants drink, they inadvertently swallow air. This medical phenomenon, known as aerophagia, is entirely normal. Because a newborn’s digestive tract is immature, those trapped air bubbles have nowhere to go. If not manually expelled through burping, the air travels down into the stomach and intestines, causing painful pressure, bloating, and excessive gas. This discomfort is a leading cause of prolonged crying spells and fussiness in infants during their first few months of life.
Furthermore, the sphincter muscle located between a baby’s esophagus and stomach is not yet fully developed. When the stomach is distended by trapped air, it pushes against this weak muscle, forcing milk back up the esophagus. Regular, effective burping reduces this pressure, thereby minimizing the frequency and volume of spit-up.
The Mechanics of a Perfect Burp
Before mastering specific positions, you must understand the physical technique required to coax air out of a tiny, delicate digestive system. The goal is to apply just enough rhythmic pressure to dislodge the air bubbles without causing the baby any pain.
The “Cupped Hand” Method
Never strike a baby’s back with a flat palm. A flat hand creates a harsh, slapping sensation that can startle or hurt the infant. Instead, gently curve your fingers inward to form a shallow cup with your hand. When you pat the baby’s back, this cupped shape creates a soft cushion of air between your hand and their body. It delivers a deeper, more hollow vibration that is highly effective at moving gas upward.
Patting vs. Rubbing
While rhythmic patting is the traditional method, firm, upward rubbing is an equally powerful tool. Starting at the lower back and applying gentle, upward strokes toward the shoulders can help manually guide the air bubbles up the esophagus. Many parents find success by alternating between three pats and a smooth, upward rub.
How Much Force is Appropriate?
First-time parents are often overly cautious, administering taps that are too light to be effective. While you should never be aggressive, you need to use firm, confident pats. Think of the pressure you would use to gently burp a small pet or tap a friend on the shoulder.
The 3 Best Burping Positions for Newborns
Every baby has a distinct anatomical preference. A technique that yields a massive burp for one infant might do absolutely nothing for another. Mastering these three primary positions ensures you have a versatile toolkit to handle stubborn gas.
1. The Over-the-Shoulder Hold
This is the classic, time-tested burping position utilized by parents and pediatricians worldwide. It relies on the firm pressure of your shoulder pressing against the baby’s stomach to force air upward.
- How to do it: Drape a burp cloth over your shoulder. Hold your baby against your chest so their chin rests comfortably on your shoulder. Ensure their tummy is pressing gently against your collarbone/upper chest area. Support their bottom with one hand while using your other cupped hand to pat or rub their back.
- Safety Tip: Always ensure the baby’s airway is completely clear and their nose is not pressed directly into your clothing.
2. Sitting Upright on the Lap
This position offers excellent visibility. You can watch your baby’s facial expressions and immediately catch any spit-up. It is highly effective for babies with severe acid reflux who need to remain completely vertical after meals.
- How to do it: Sit the baby upright on your thigh, facing sideways or away from you. Lean them slightly forward. Use the heel of your supporting hand to support their chest, and lightly grip their jaw and chin with your thumb and index finger. Do not grip their throat. Use your free hand to pat their back.
- Pro Tip: Gently rocking the baby back and forth or moving their torso in a slow, circular motion while in this position can help dislodge stubborn air pockets before you begin patting.
3. Face Down Across Your Lap
If your baby is exhausted and falling asleep, or if the first two positions have failed, this gravity-assisted method is an excellent alternative.
- How to do it: Lay the baby stomach-down across your knees, perpendicular to your body. Position them so their tummy rests on one leg and their head is supported by the other leg. Ensure their head is turned sideways and elevated slightly higher than their chest to prevent blood from rushing to their head. Pat or rub their back firmly.
Position Comparison Guide
| Burping Position | Pros | Cons | Best Used For |
| Over the Shoulder | Highly intuitive; comforting for the baby; allows for easy walking/bouncing. | Difficult to see the baby’s face; high risk of spit-up on your back/clothes. | Newborns lacking head control; fussy babies who need body contact. |
| Sitting Upright | Keeps the baby fully vertical; easy to monitor breathing and spit-up. | Requires careful hand placement to avoid the throat; can be awkward at first. | Babies with acid reflux; older infants with slight neck strength. |
| Face Down on Lap | Gravity assists gas expulsion; gentle pressure on the tummy relieves cramps. | Baby may dislike being placed on their stomach; harder to comfort if crying. | Sleepy babies; stubborn, trapped gas that won’t move. |
When and How Often Should You Burp Your Baby?
The frequency of your burping sessions depends heavily on how your baby is fed. The mechanics of drawing milk from a breast versus a silicone nipple dictate how much air is swallowed.
Bottle-Fed Babies: Bottle feeding generally introduces more air into the stomach because air naturally gets trapped inside the bottle, and the flow rate is often faster than a breast. You should aim to burp a bottle-fed baby after every 2 to 3 ounces of formula or breastmilk. If your baby is a rapid eater, pause them more frequently. Exploring specialized anti-colic bottles and soothing infant essentials can significantly reduce the amount of air your baby swallows in the first place, making the burping process much easier.
Breastfed Babies:
A proper latch creates a vacuum seal, meaning breastfed infants typically swallow far less air. However, they are not immune to gas. The standard recommendation is to burp a breastfed baby every time they switch breasts. If your baby only feeds on one side per session, burp them halfway through the feed and again when they unlatch completely.
Reading the Signs: How Do You Know They Need to Burp?
Babies cannot tell you when they are uncomfortable, but their body language speaks volumes. If you observe any of the following behaviors during or immediately after a feeding, it is time to pause and switch to a burping position:
- Pulling Away: Repeatedly unlatching from the breast or aggressively turning their head away from the bottle, only to root around for it seconds later.
- Squirming and Arching: A baby experiencing painful gas will often arch their back rigidly, stiffen their legs, and squirm uncontrollably in your arms.
- Grimacing: Watch for tightened lips, furrowed brows, or a pained expression.
- Fussiness: Sudden, unexplained crying mid-feed is almost always a sign of trapped air.
What to Do When the Baby Won’t Burp
It is a common scenario: you have been patting your baby’s back for ten minutes, your arm is exhausted, and there is no burp in sight. First, do not panic. Not every feeding results in a burp. If your baby seems perfectly content and relaxed, they likely didn’t swallow enough air to require burping. You can safely lay them down or resume feeding.
However, if they are clearly uncomfortable and the burp is “stuck,” you must switch tactics:
- Change Positions: Move them from your shoulder to a sitting position. Sometimes, the simple act of lifting and shifting their body is enough to un-kink the digestive tract and release the air.
- Bicycle Legs: Lay the baby flat on their back. Gently take their ankles and cycle their legs in a pedaling motion toward their stomach. This physically massages the intestines and forces lower gas out.
- Tummy Time Massage: Laying your baby on their stomach (while awake and supervised) naturally compresses the abdomen. Gently rubbing their back while they are in this position can work wonders.
- Take a Break: Stop forcing it. Hold the baby upright against your chest, rock them for 5 to 10 minutes, and then try burping again.
Managing the Inevitable Spit-Up
When the burp finally comes, it frequently brings milk along for the ride. This is called a “wet burp,” and it is an unavoidable reality of early parenthood. Because the esophageal valve is loose, air pushing upward will naturally carry whatever liquid is sitting on top of the stomach.
Preparation is your only defense. Never initiate a burping session without protection. Investing in high-quality, absorbent burp cloths and protective feeding gear is crucial to saving your clothing and furniture from constant stains. Drape the cloth widely over your shoulder or lap before you even pick the baby up. If your baby is a “happy spitter” (meaning they spit up frequently but are gaining weight and not in pain), this is a laundry issue, not a medical one.
Building a support network and gathering reliable information can drastically reduce the anxiety associated with newborn feeding issues. Exploring community tips and expert resources on the Wobblebee homepage can provide you with peace of mind and practical advice from parents who have navigated the same challenges.
Frequently Asked Questions
How long should I try to burp my baby?
You should try burping your baby for about 5 to 10 minutes. If they have not burped after that time and appear comfortable, you can stop and resume feeding or lay them down to sleep.
Do breastfed babies need to be burped?
Yes, breastfed babies still need to be burped, though they typically swallow less air than bottle-fed babies. It is best practice to burp them whenever you switch breasts or at the end of a feeding.
What if my baby falls asleep before burping?
If your baby falls asleep while feeding, try burping them gently using the over-the-shoulder or face-down-on-lap position. If they don’t burp after a few minutes and are sleeping peacefully, it is safe to place them in their crib on their back.
When can I stop burping my baby after feedings?
Most babies naturally outgrow the need for manual burping between 4 and 6 months of age. As their digestive systems mature and they spend more time sitting upright, they become capable of expelling gas on their own.
Why does my baby scream when I try to burp them?
Crying during burping can be caused by severe trapped gas that is painful to move, or it may indicate acid reflux, where stomach acid is irritating the esophagus. If your baby consistently screams in pain during burping, consult your pediatrician to rule out reflux or food intolerances.





